In order to prevent, treat, or cure diseases, scientists rely on methods for identifying consistent mechanisms behind disease, and efficiently testing potential therapies on a broad scale. A central goal of Project ALS has been to support research efforts that develop tools for studying ALS disease mechanisms, and therefore have long-term promise in the development of future therapies, diagnostics, and potential cures. ALS has been a historically difficult disease to study, treat, and cure because of its variability in onset and disease progression across those living with ALS, and its primary impacts on aging motor neurons in the spinal cord and brain that are difficult to observe and access. In 2002, however, the possibilities for ALS research completely changed thanks to the development of a breakthrough method: motor neurons in a dish.
Method Born in 2002: From in vivo to in vitro
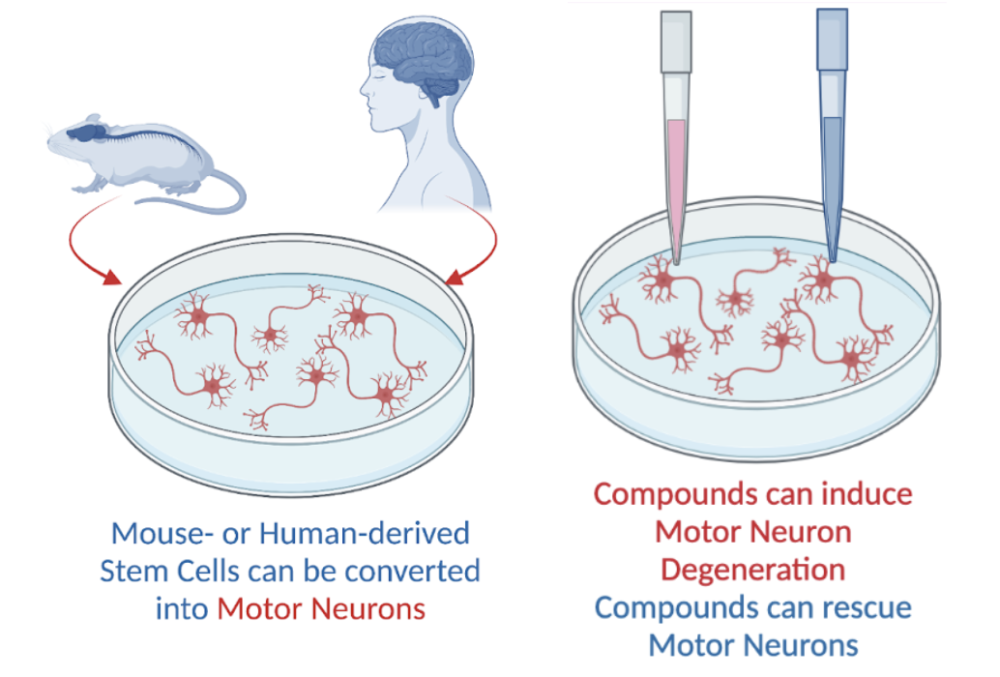
Previous ALS research relied on investigating motor neuron degeneration and testing potential therapies in mouse models alone, or in vivo. While this type of approach can be beneficial for understanding ALS and testing its potential treatments in a way that more closely resembles human physiology, in vivo techniques can be time-consuming, difficult to perform in large numbers, and require complicated techniques for observing motor neuron health directly.
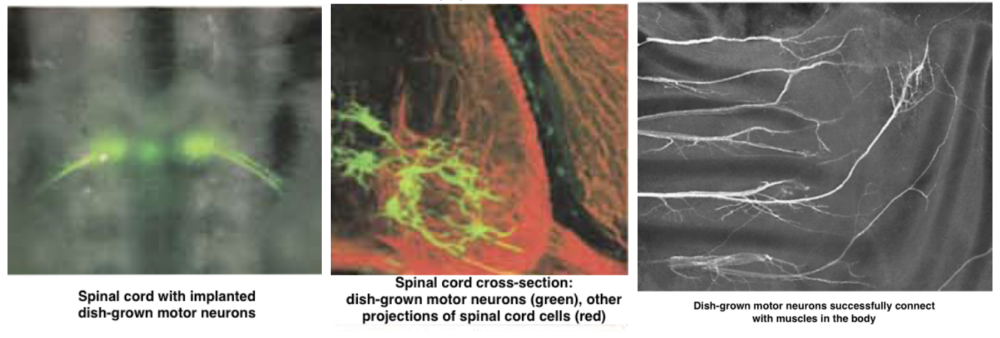
Hynek Wichterle—now a Project ALS Therapeutics Core Co-Scientific Director—and his colleagues in the Jessell lab at Columbia University, realized twenty years ago that the ability to grow, observe, and manipulate motor neurons outside of the body would allow for more detailed and rapid progress in understanding what happens to motor neurons in ALS and testing therapeutic compounds on a massive scale. Wichterle cleverly harnessed findings from developmental research to grow realistic motor neurons rapidly and in large numbers in a dish, or in vitro. Specifically, Wichterle exposed mouse embryonic stem cells—”blank slate” cells that have not yet acquired a specific function or identity, like muscle cell, cardiac cell, or neuron—to the specific sequence of molecules that developing motor neurons are exposed to. Then, Wichterle and colleagues tested how realistically these in vitro motor neurons mimic in vivo motor neurons. They demonstrated that dish-grown motor neurons expressed the same genes that in vivo motor neurons express. Further, as seen in the image below, dish-grown motor neurons can successfully incorporate themselves into developing spinal cords and connect with muscles in the body, just like in vivo motor neurons.
Motor Neurons in a Dish in 2022: The Next Generation of In Vitro ALS Research
Thanks to the efforts of Project ALS in promoting this type of methodological research, motor neurons in a dish have profoundly impacted how researchers currently study the mechanisms of degeneration in and test potential therapies for ALS faster and in greater detail than ever before. Thanks to this groundbreaking work, researchers went on to develop additional stem cell-based methods for studying ALS motor neurons in a dish: from generating motor neurons from skin samples of people with ALS in 2008, to developing methods that induce motor neuron degeneration that closely mimics ALS disease progression in a dish in 2018. These exact tools have since paved the way for the development of promising therapeutic compounds, including Kenpaullone and the Project ALS Therapeutics Core’s first investigational drug, prosetin, now in clinical trials. Finally, recent work from 2019 supported by Project ALS that capitalizes on in vitro motor neuron techniques has uncovered a new mechanistic understanding of why specific types of motor neurons are more susceptible to degeneration during ALS disease progression, yielding another potential avenue for treating ALS, or even preventing ALS onset in the near future.